Osteoarthritis affects millions of people worldwide. It occurs when the protective cartilage, cushioning the ends of the bones, wears down over time.
Although this disease can damage any joint, the most commonly affected joints are the knees, hands, hips, and spine.
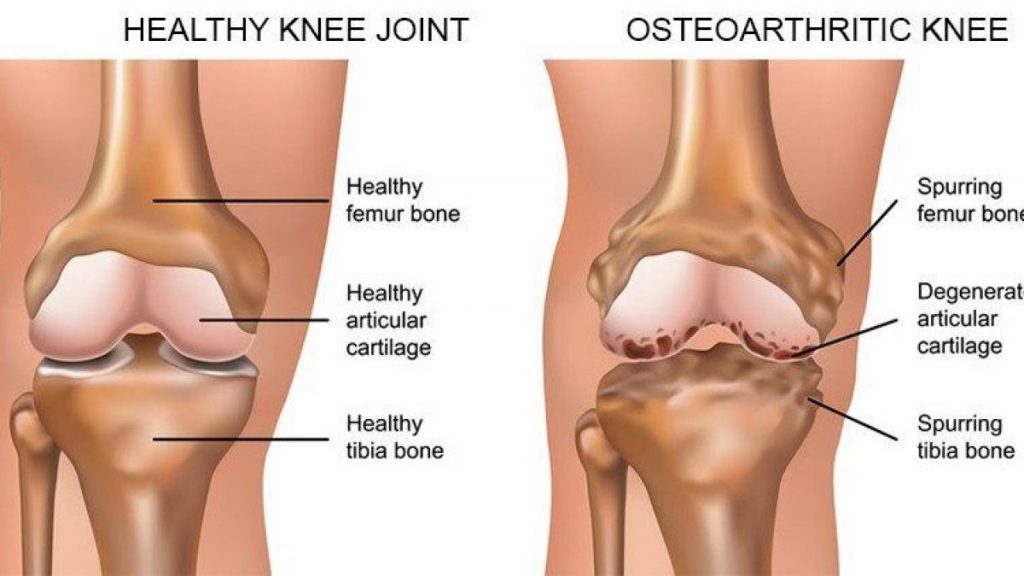
Signs & symptoms of osteoarthritis may develop slowly and worsens over time. Examples include :
If you have any of the symptoms above, make an appointment to see a doctor.
As you get older, you are at a higher risk of osteoarthritis. Women, however, are more likely to get it.
Moreover, being obese adds stress to the joint and thus, may increase the risk this disease.
This disease can also be hereditary.

Over time, osteoarthritis may worsen. Joint pain and stiffness might become severe enough to make daily tasks difficult. Hence, this may cause some people to be unable to perform daily tasks.
Osteoarthritis can’t be fully prevented. However, you can try reducing the risk by reducing stress on the joints. For example:
Extra weight can cause stress on the joints. Additionally, extra fat will also cause changes in the cartilage.
High blood sugar level increases the risk for osteoarthritis.
Exercise not only can prevent joint problems by keeping joints from getting stiff, but it can also keep muscles strong.
In a nutshell, prevention and treatment of osteoarthritis are possible. Here at Mayflax, we provide various types of drugs for various diseases. Contact us here to get to know us better

Epilepsy, a common neurological disease, is a chronic disorder that causes repetitive seizures.
A seizure is a sudden rush of electrical activity in the brain.
There are two types of seizures; generalized seizures and focal seizures.
Generalized seizures affect the whole brain while focal seizures affect just one part of the brain.
Epilepsy is caused by abnormal activity in the brain. Sign and symptoms include:
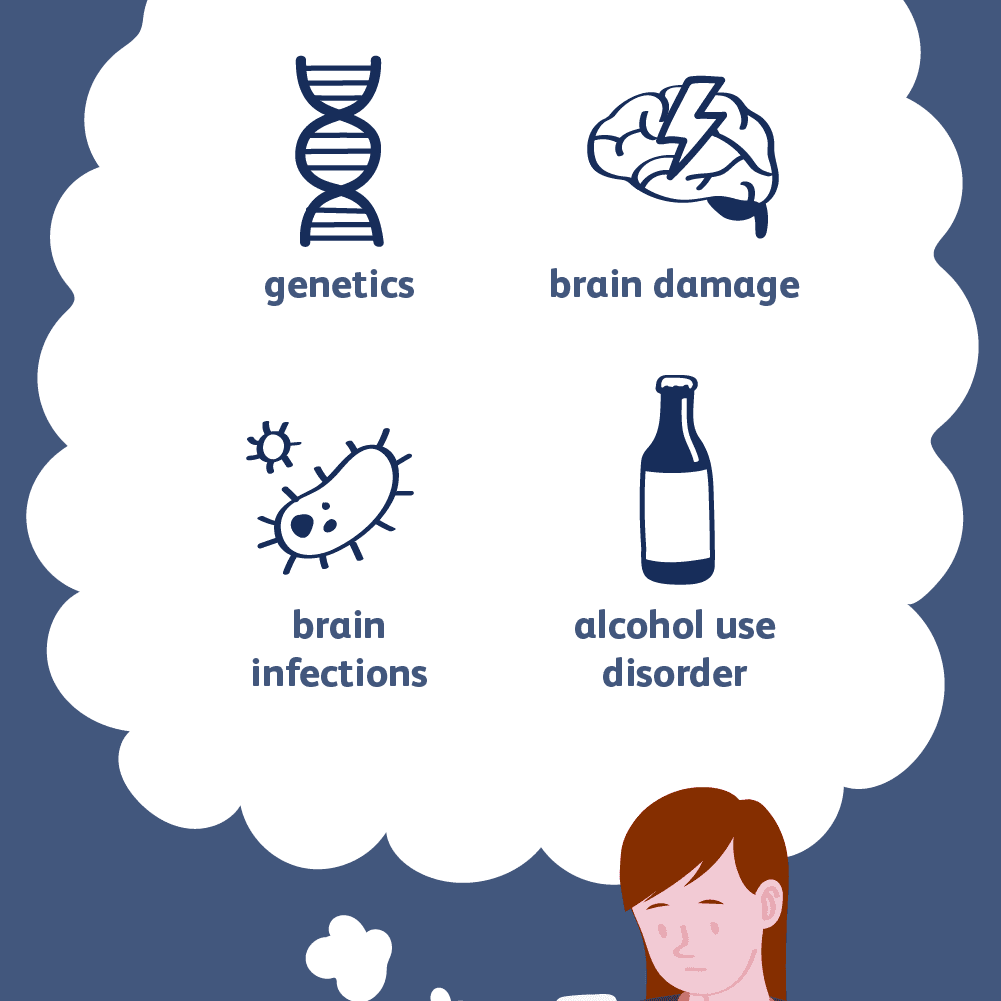
The risk of having epilepsy may be increased by certain factors, namely:
This disease, like many other diseases, comes with several complications.
Seizures at certain times may be dangerous to patients and to others.
For instance, the likelihood of falling during a seizure attack is high. Falling during a seizure may injure the head.
Epileptic patients are also more likely to drown while bathing or swimming.
Moreover, epilepsy during pregnancy may pose danger to both the mother and the fetus.
To add, a certain anti-epileptic drug may increase the risk of birth defects. Discuss with your doctor before planning to get pregnant.
On the other hand, people with epilepsy tend to get psychological problems, such as depression, and anxiety. This is because of the difficulties dealing with the condition itself and medication side effects.

Several types of treatments exist to treat this disease.
Most commonly patients are treated with oral medications, called anti-epileptic drugs.
However, if oral medications fail to give desirable effect, another type of treatment is also available, such as:
Mayflax has 25 years of experience and provides over 2000 pharmaceutical products at low prices too!
If you want to use our service as a supplier, feel free to contact us here.
Gout is a common form of arthritis. It is also a painful condition that usually involving the joints. It is caused by high levels of uric acid in the blood. Uric acid is formed when the body breaks down purines. The purines can be found in the body and certain foods. When symptoms get worse, it is known as flares. When there are no symptoms, it is known as remissions.

There are many risk factors for gout.Gout generally develops in men between age 30 to 45 and women age 55 to 70.
Increased Risk for Developing Gout:
Gout occurs when there is an excess of uric acid in the body. The body makes uric acid when it breaks down purines. Purines are found in the body and the foods we eat. Usually, uric acid crystals can build up in joints, fluids, and tissues within the body when there is an excess of uric acid in the body. Hyperuricemia does not always cause gout. In addition, hyperuricemia without gout symptoms does not need to be treated. The sharp, needle-like crystals cause gout.
Symptoms develop quite rapidly. It can last for three to ten days. Usually, the symptoms and signs affect a single joint. Gout attacks are very painful. It can happen quite suddenly, often overnight. The pain is typically severe. So, it shows the severity of inflammation in the joint. The medical term for excessive fluid in a joint is a “joint effusion”.

Pseudogout also is a form of arthritis that causes sudden joint pain and swelling. It is caused by calcium pyrophosphate dihydrate crystals (CPPD).
The sudden attacks of joint pain, swelling, and warmth can occur when you have pseudogout. It can last for days to weeks. It can affect the ankles, feet, shoulders, elbows, wrists, or hands but it mostly affects the knee.
Besides older age, several other factors also increase the risk for developing pseudogout :
Pseudogout occurs when calcium pyrophosphate crystals form in the synovial fluid in the joints. Crystals can also deposit in the cartilage and can cause damage. The formation of crystal in the joint fluid results in swollen joints and acute pain. Older people have higher possibilities of getting pseudogout compared to younger people. In addition, the genetic condition can cause pseudogout because it always occurs in families.
In addition, other factors may include :
Pseudogout most often affects the knees. In addition, it also affects the ankles, wrists, and elbows.
General symptoms may include:

Until now, no treatment can completely remove or prevent the formation of calcium pyrophosphate dehydrate crystals. Therefore, treatment is generally focused on reducing pain and swelling.

Nur Ayuni Mohd Ruduan, Bachelor of Science (Hons) Pharmacology, is staff officer of Mayflax, one of the nation’s leading healthcare and marketing company.
Based on a study, survival rate in patients with COVID-19 was improved with the use of colchicine, which are usually used for the treatment of gout and other inflammatory disorders as compared with standard of care (SoC).
The well-recognised anti-inflammatory effects and potential antiviral properties made it as one of the drugs that was considered for the treatment of COVID-19. 140 hospitalized patients who contracted COVID-19 had their outcomes evaluated as they were treated with SoC (hydroxychloroquine and/or intravenous dexamethasone; and/or lopinavir/ritonavir) and in 122 patients treated with colchicine and SoC.
The SoC group, have lower serum concentrations of C-reactive prottein and ferritin, as well as neutrophil count but higher PaO2/FiO2 ratio at baseline.
Survival when being compared over 21 days of follow-up, it was more favourable in the colchicine than the SoC group. A lower risk of death was strongly associated with colchicine, on Cox proprortional hazards regression (hazard ratio, 0.151).
At entry, there were a higher serum levels of ferritin, worse Pa02/Fi02 and poor survival at older age for the risk factors.
With no treatment discontinuation due to severe adverse events, colchicine had a good safety profile. In nine patients, dosing was reduced from 1 to 0.5 mg/day due to diarrhoea.
With the aim of preventing the patient’s autoinflammatory response, the current study provides proof-of-concept data supporting the possible use of colchicine in the treatment of the early phase of COVID-19.
To determine the efficacy and safety of colchicine, properly designed trials are needed with the best protocol in terms of dosage and timing of administartion in patients with COVID-19, said the researchers.
Share the post!
Mon to Fri: 8:00am to 5:00pm
Sat: 8:30am to 12:30pm


